 A new study published in the Journal of Clinical Sleep Medicine has found that a group of men with obstructive sleep apnea who also had high blood pressure, benefited from a significant lowering of their blood pressure when their sleep apnea was treated with a form of positive airway pressure (PAP) therapy.
A new study published in the Journal of Clinical Sleep Medicine has found that a group of men with obstructive sleep apnea who also had high blood pressure, benefited from a significant lowering of their blood pressure when their sleep apnea was treated with a form of positive airway pressure (PAP) therapy.
Obstructive sleep apnea creates pauses in breathing during the night and disrupts sleep. According to the National Library of Medicine, National Institutes of Health, “Obstructive sleep apnea is a condition in which the flow of air pauses or decreases during breathing while you are asleep because the airway has become narrowed, blocked, or floppy.”
The new study, by Bharati Prasad, M.D., M.S. of the Department of Medicine, University of Illinois at Chicago, IL, and colleagues, was published in the October 15, 2012 online issue of the Journal of Clinical Sleep Medicine, a journal of the American Academy of Sleep Medicine.
The Study; Method
The study included 221 men who had preexisting hypertension (high blood pressure) or type 2 diabetes, and who were newly diagnosed with obstructive sleep apnea.
The participants were prescribed and received positive airway pressure (PAP) therapy to treat their sleep apnea.
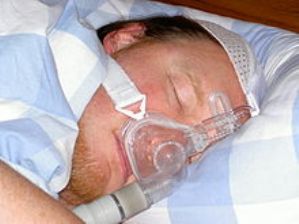
According to the Stanford Center for Sleep Sciences and Medicine,”Positive airway pressure (PAP) Therapy is a generic term applied to all sleep apnea treatments that use a stream of compressed air to support the airway during sleep. With PAP therapy, you wear a mask during sleep. A portable machine gently blows pressurized room air from into your upper airway through a tube connected to the mask. This positive airflow helps keep the airway open, preventing the collapse that occurs during apnea, thus allowing normal breathing.”
The men were tested at 3 to 6 months and again at 9 to 12 months after starting the PAP therapy, to see if there were any changes in their blood pressure (systolic and diastolic) or glycemic control (measured by fasting glucose and hemoglobinA1C values).
Findings
The researchers found significant decreases in both systolic and diastolic blood pressure readings in the men both at 3 to 6 months after starting the PAP therapy, and again when re-tested at 9 to 12 months after starting the treatment.
The results remained significant after adjusting for potential confounding factors, including demographics, body mass index (BMI), severity of obstructive sleep apnea, and pharmacologic treatment for hypertension and diabetes.
However, “Diabetes control measures did not change with OSA [obstructive sleep apnea] treatment,” the researchers found.
Conclusions; Implications
The results indicate that, for men with obstructive sleep apnea and high blood pressure, PAP therapy may be an effective way to treat not only their sleep disorder, but also their hypertension, the study authors reported.
“All types of patients may benefit from this treatment, even those with other chronic medical conditions,” Dr. Bharati Prasad, the study’s principal author, said in a news release issued by the American Academy of Sleep Medicine.
“It’s important to now do a prospective study enrolling different types of patients with sleep apnea,” he continued.
While the study found an association between reductions in high blood pressure levels and PAP therapy for sleep apnea, it did not prove an actual cause-and-effect relationship.
More Information
For more information on high blood pressure, see the HelpingYouCare® resource pages on High Blood Pressure, including:
- Latest News on High Blood Pressure;
- What is it; Causes;
- Symptoms & Diagnosis;
- Prevention;
- Treatment;
- Caregiving.
For more information on the importance of sleep and other lifestyle factors for wellness and disease prevention, see the HelpingYouCare® resource pages on Wellness/ Healthy Living for Seniors & Caregivers, including:
- Diet & Nutrition: Physical Wellness;
- Exercise: Physical Wellness;
- Sleep, Hygiene, Quit Smoking & Other Healthy Practices: Physical Wellness;
- Activities to Preserve Mental Acuity: Intellectual Wellness;
- Social Interaction & A Sense of Connection With Others: Social Wellness;
- Other Areas of Wellness: Emotional, Ethical/ Spiritual & Vocational Wellness; and
- Healthy Living: Stories of Inspiring Seniors.
_____________
Copyright © 2012 Care-Help LLC, publisher of HelpingYouCare®. All rights reserved.
NOTICE: If you are reading this article on any website other than HelpingYouCare.com, please click HERE to go to the original article. No website other than HelpingYouCare® has been given permission to publish this article.



