 The American Medical Association (AMA), the largest and primary professional organization of medical doctors in the U.S., passed a resolution at their annual meeting on June 18, officially declaring that obesity shall be recognized as a disease.
The American Medical Association (AMA), the largest and primary professional organization of medical doctors in the U.S., passed a resolution at their annual meeting on June 18, officially declaring that obesity shall be recognized as a disease.
The AMA had previously categorized obesity as a “related condition” or “disorder,” and recognized it as “a major public health problem contributing to 112,000 preventable deaths each year,” but by its action last Tuesday, the AMA has “upgraded” obesity to the status of a “disease.”
This move highlights the serious medical consequences of obesity, and may encourage health insurance companies to cover obesity counseling and treatment and reimburse doctors for their services in helping obese patients, according to news reports about the matter.
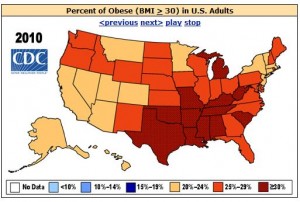 This AMA action could affect a huge swath of Americans. Data provided by the U.S. Centers for Disease Control & Prevention (CDC) indicate that “More than one-third of U.S. adults (35.7%) are obese” (measured by having a body mass index (BMI) of more than 30).
This AMA action could affect a huge swath of Americans. Data provided by the U.S. Centers for Disease Control & Prevention (CDC) indicate that “More than one-third of U.S. adults (35.7%) are obese” (measured by having a body mass index (BMI) of more than 30).
“In 2009–2010, over 78 million U.S. adults and about 12.5 million U.S. children and adolescents were obese,” according to the data cited by the CDC.
A report entitled titled “F as in Fat: How Obesity Threatens America’s Future 2012,” issued in September, 2012 by the nonprofit Trust for America’s Health and Robert Wood Johnson Foundation, projects that if current trends continue, by 2030, more than 50% of adults could be obese in 39 U.S. States, 13 states could have adult obesity rates above 60 percent, and all 50 states would have obesity rates of more than 44 percent.
The resolution, passed by a vote of the AMA’s House of Delegates on Tuesday — with approximately 60% voting in favor, states, in part:
“We felt it’s time to take a stance and say we’re going to identify this as a disease,” Dr. Douglas Martin, chairman of the AMA public health committee that referred the resolution for the vote of the AMA House of Delegates, told MedPage Today. “We think that’s going to send a message not only to the public but to the physician community that we really need to make it a priority and put it in our cross hairs.”
A press release issued by the AMA quoted AMA board member Patrice Harris, M.D. as saying, “Recognizing obesity as a disease will help change the way the medical community tackles this complex issue that affects approximately one in three Americans.”
“The AMA is committed to improving health outcomes and is working to reduce the incidence of cardiovascular disease and type 2 diabetes, which are often linked to obesity,” Dr. Harris said.
Recognized Health & Economic Consequences of Obesity
According to the CDC, “Obesity-related conditions include heart disease, stroke, type 2 diabetes and certain types of cancer, some of the leading causes of preventable death.”
More specifically, the CDC reports, “Research has shown that as weight increases to reach the levels referred to as “overweight” and “obesity,” the risks for the following conditions also increases:
- Coronary heart disease
- Type 2 diabetes
- Cancers (endometrial, breast, and colon)
- Hypertension (high blood pressure)
- Dyslipidemia (for example, high total cholesterol or high levels of triglycerides)
- Stroke
- Liver and Gallbladder disease
- Sleep apnea and respiratory problems
- Osteoarthritis (a degeneration of cartilage and its underlying bone within a joint)
- Gynecological problems (abnormal menses, infertility).”
“Overweight is defined as a body mass index (BMI) of 25 or higher; obesity is defined as a BMI of 30 or higher,” the CDC explains. The CDC also provides more information on Defining Obesity.
“In 2008, medical costs associated with obesity were estimated at $147 billion; the medical costs for people who are obese were $1,429 higher than those of normal weight,” the CDC reports.
According to the latest report by the Trust for America’s Health and Robert Wood Johnson Foundation (referenced above), if current trends continue, “The number of new cases of type 2 diabetes, coronary heart disease and stroke, hypertension and arthritis could increase 10 times between 2010 and 2020 — and then double again by 2030; and Obesity-related health care costs could increase by more than 10 percent in 43 states and by more than 20 percent in nine states.”
However, “if we could lower obesity trends by reducing the average adult BMI (body mass index) by only 5 percent in each state, we could spare millions of Americans from serious health problems and save billions of dollars in health spending — between 6.5 percent and 7.8 percent in costs in almost every state,” the report states.
Current Tax and Insurance Treatment of Obesity
The Internal Revenue Service has held that obesity treatments can qualify for tax deductions, according to reporting by the New York Times.
In 2004, Medicare removed language from its coverage manual saying obesity was not a disease, the NY Times reports. As we reported in September, 2011, “The U.S. Centers for Medicare and Medicaid Services (CMS) issued a proposed Decision Memorandum on August 31, 2011, recommending that seniors who have Medicare Part A or Part B should be covered for an obesity screening, dietary assessment, and, if indicated, intensive behavioral counseling in diet and exercise and behavioral therapy to promote sustained weight loss.” These services would need to be provided by a “primary care physician” or “primary care practitioner” (nurse practitioner, clinical nurse specialist, or physician assistant) in a “primary care setting.”
“Still, Medicare Part D, the prescription drug benefit, includes weight loss drugs among those it will not pay for, along with drugs for hair growth and erectile dysfunction,” according to the NY Times.
“But coverage for such obesity treatments has been uneven among private insurers,” according to reporting by the Los Angeles Times.
Pros and Cons of the AMA’s Position
In voting to recognize obesity as a disease, the medical doctors who are members of the AMA overrode a recommendation of the AMA Council on Science and Public Health, which had studied the issue over the past year, and after considering a list of pros and cons in defining obesity as a disease, had recommended against adoption of the measure.
The Council concluded that obesity should not be considered a disease, mainly on the grounds that the measure currently used to define obesity (having a body mass index (BMI) above 30) is simplistic and flawed — meaning that some people with a BMI above 30 can be perfectly healthy, while others with a BMI below 30 can experience the metabolic problems and dangerous levels of body fat associated with obesity.
“Why should a third of Americans be diagnosed with a disease if they’re not necessarily sick?” council member Robert Gilchick, MD, MPH, said in remarks made to MedPage Today.
Among the factors in favor of defining obesity as a disease, the Council cited a likelihood that doing so may reduce the stigma associated with obesity, which stems from a widespread perception that it is simply the result of eating too much or exercising too little, factors within a person’s control. Some doctors, however, point out that other health conditions or medications can impact weight, and say that people in fact do not have full control over their weight.
Those opposed to recognizing obesity as a disease, “say that “medicalizing” obesity by declaring it a disease would define one-third of Americans as being ill and could lead to more reliance on costly drugs and surgery rather than lifestyle changes,” according to reporting by the New York Times. This could result in some people being overtreated because their B.M.I. is above 30, even though they may be healthy, opponents argued.
In its report, the AMA’s Council wrote:
Nevertheless, approximately 60% of the AMA’s members rejected the conclusions of the AMA’s Council, and voted in favor of the resolution recognizing obesity as a disease.
The resolution was backed by delegates from several other recognized medical associations and societies, including the American Academy of Pediatrics, the American Academy of Family Physicians, the American Association of Clinical Endocrinologists, and the American Society of Bariatric Physicians.
In a statement issued June 19, the American Heart Association (AHA) lauded the AMA’s decision to identify obesity as a disease, saying that “The American Heart Association believes the additional focus is needed on this important risk factor for heart disease and stroke.”
Implications
The AMA has no legally binding authority to cause insurers to cover obesity treatment. Nor is the AMA the final arbiter of what constitutes a “disease.” In fact, with respect to the labeling of diseases internationally, the World Health Organization (WHO) provides the International Classification of Diseases (ICD), which already includes a range of coded disease categories for obesity. These include:
- E66.0 Obesity due to excess calories
- E66.1 Drug-induced obesity
- E66.2 Extreme obesity with alveolar hypoventilation (Pickwickian syndrome)
- E66.8 Other obesity (Morbid obesity)
- E66.9 Obesity, unspecified (Simple obesity NOS)
According to reporting by the New York Times, “some doctors and obesity advocates said that having the [U.S.] nation’s largest physician group make the declaration [that obesity shall be recognized as a disease] would focus more attention on obesity. And it could help improve reimbursement for obesity drugs, surgery and counseling.”
“I think you will probably see from this physicians taking obesity more seriously, counseling their patients about it,” Morgan Downey, an advocate for obese people and publisher of the online Downey Obesity Report, told the New York Times.
More Information
For a presentation of additional statistics on the extent of obesity in America, see a graphic by NPR, entitled “Obesity In America, By The Numbers.”
See related HelpingYouCare® reports on:
More than 50% Obesity in 39 States by 2030, New F as in Fat Report Projects
CDC Teaches that Healthy Weight is a Lifestyle – Not Just a Diet
New HBO Documentary, The Weight of The Nation, Explores Causes, Costs of Obesity
New Reports Document High Costs of Obesity in America
Medicare Recommends Coverage of Seniors for Intense Obesity Counseling
Obesity Alert: Scientists Warn of Alarming Health Costs, Discuss Cures
The Obesity Epidemic: What it Means for America & What Can Be Done About It
Diabetes Pandemic Linked to Obesity Epidemic; Study Finds Early Diet Intervention Helps
For more information on maintaining a healthy weight, healthy diet, exercise and other lifestyle factors that promote wellness and prevent diseases, see the HelpingYouCare® resource pages on Wellness/ Healthy Living for Seniors & Caregivers, including:
- Weight Loss/ Maintaining a Healthy Weight: Physical Wellness;
- Diet & Nutrition: Physical Wellness;
- Exercise: Physical Wellness;
- Sleep, Hygiene, Quit Smoking & Other Healthy Practices: Physical Wellness;
- Activities to Preserve Mental Acuity: Intellectual Wellness;
- Social Interaction & A Sense of Connection With Others: Social Wellness;
- Other Areas of Wellness: Emotional, Ethical/ Spiritual & Vocational Wellness; and
- Healthy Living: Stories of Inspiring Seniors.
_____________
Copyright © 2013 Care-Help LLC, publisher of HelpingYouCare®. All rights reserved.



