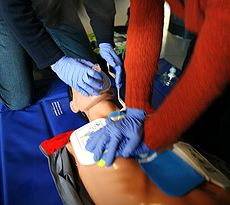
 A new study published in the March 14 New England Journal of Medicine has found that family members who are invited to be present during the quite brutal and aggressive cardiac resuscitation procedures performed as a last-ditch life-saving effort when a patient goes into cardiac arrest, actually suffer less psychological trauma from the event than family members who are excluded.
A new study published in the March 14 New England Journal of Medicine has found that family members who are invited to be present during the quite brutal and aggressive cardiac resuscitation procedures performed as a last-ditch life-saving effort when a patient goes into cardiac arrest, actually suffer less psychological trauma from the event than family members who are excluded.
The new study, conducted by an international team of researchers including a lead author Patricia Jabre, M.D., PHD, of the Department of Health Sciences Research at the Mayo Clinic, Rochester, Minnesota, and colleagues, entitled “Family Presence during Cardiopulmonary Resuscitation,” was published on March 14, 2013 in the New England Journal of Medicine.
On the same date, the New England Journal of Medicine has published a Case Vignette describing a 72-year-old hospitalized woman whose pulse stops and who goes into cardiac arrest, requiring the medical team to administer chest compressions and cardiopulmonary resuscitation, starting at the moment when the patient’s husband and two children arrive.
The Journal invites its readers, primarily medical professionals, to respond to a poll as to whether the physicians should invite the husband and children to be present during the resuscitation efforts or not. Specifically, the Journal asks its readers to comment on which of two proposed approaches the physicians should take:
To explain the two alternative approaches, the Journal publishes short summaries by two experts in the field — one arguing for family presence during Resuscitation, and the other against it. The experts’ views, as well as the findings of the new study, are summarized further below.
The Journal’s readers, primarily physicians, have until March 20, 2013 to submit their votes and comments. So far, the comments published have voted for the two alternatives presented in approximately equal numbers.
The Case Vignette, entitled, “Family Presence during Cardiac Resuscitation,” and poll with comments was published in the New England Journal of Medicine, March 14, 2013.
Strikingly, nearly all of the comments published in the Journal so far were submitted by physicians who argue for or against allowing family to be present on the basis of whether, in the physician’s experience, presence of family members may be disruptive to the medical team and/ or whether the physician believes that witnessing the quite brutal and aggressive shocks and blows to the patient’s chest that occur during resuscitation efforts may be psychologically disturbing or traumatic to the family members.
At the time of this writing, only two of the comments were submitted by family caregivers (one of whom appears also to have been possibly a medical student). Both came down on the side of inviting and allowing family members to be present. Their moving comments are quoted below:
[Submitted by "JM | Category: Student"] “Aside from the time in the operating room, I was personally present each time my father had gone into cardiac arrest the night he passed away. From the very beginning that night, he had been in serious condition. The staff had encouraged my family and me to leave each time CPR was being done, but I didn’t want my father to pass away without a loved one being by his side. So I personally took upon that role and stayed while the rest of my family sat outside. I didn’t try to intervene with the CPR efforts, I didn’t tell the staff what to do, I just stood and watched. I witnessed all of it, each painful compression that my father sustained. Despite all the sedation, anesthetics and the attending’s reassurance that he didn’t feel pain, in some sense, I’m positive he felt each of those compressions. I just can’t fathom how such force can’t be felt. It was painful for me to watch, and to this day, I still replay what I saw in my head. But I do not suffer from PTSD. And I do not regret being present during his cardiac arrest. I am so glad that I was there so that if he were to pass, I would be by my father’s side, and he wouldn’t have been alone.”
What is your opinion as a family caregiver? We invite you to login and submit your comments below.
What The Experts Say
In Favor of Inviting Family Members to be Present During Resuscitation
Patricia A. Kritek, M.D., citing source information from the Division of Pulmonary and Critical Care Medicine, University of Washington Medical Center, Seattle, and also citing the new study by Dr. Jabre, and colleagues, published on March 14, 2013 in the New England Journal of Medicine, argues for allowing family members to observe resuscitation efforts.
Dr. Kritek states that the patient’s “family deserves the opportunity to be in the room in what may be the last minutes of her life.”
She notes that some “Small observational studies in the 1990s raised concerns that watching a loved one undergo CPR might result in immediate distress and lingering psychological impact.”
However, she reports that “More recent studies, including the large, randomized, controlled trial reported in this issue of the Journal, show the opposite; in the study by Jabre et al., relatives who did not witness resuscitation efforts were more likely to have anxiety, depression, and PTSD-related symptoms afterwards.”
As noted, the study referred to by Dr. Kritek, entitled “Family Presence during Cardiopulmonary Resuscitation,” and conducted by Patricia Jabre, M.D., PHD, of the Department of Health Sciences Research at the Mayo Clinic, Rochester, Minnesota, and colleagues, was also published on March 14, 2013 in the New England Journal of Medicine.
In that study, 570 relatives of patients who were in cardiac arrest and were given CPR by 15 prehospital emergency medical service units were randomly assigned to two groups. In one of the groups (identified as the “intervention group”), the family members were invited to observe CPR efforts on the patient. In the other group (the “control group”), the standard medical practice of excluding family members from the room where CPR is performed was followed.
The researchers found that “the frequency of PTSD-related symptoms was significantly higher in the control group [the family members who did not witness the CPR procedure] than in the intervention group [in which the family members did observe the CPR efforts].
The authors of that study concluded that, “Relatives who did not witness CPR had symptoms of anxiety and depression more frequently than those who did witness CPR.” They also found and concluded that “Family-witnessed CPR did not affect resuscitation characteristics, patient survival, or the level of emotional stress in the medical team and did not result in medicolegal claims.”
As to concerns that family presence may impede or interfere with performance of the medical team, Dr. Kritek cites “more recent research, including the study by Jabre et al., [which] shows that providers can perform equally well and feel equally comfortable with or without the family present.”
She advocates having a trained family liaison present to explain to the family members what is occurring during the resuscitation efforts and to help guide them through the emotional experience. This, she says, plus proper training of the medical team, has been shown to ease concerns of the medical professionals and help them become comfortable with family members being present.
Dr. Kritek concludes, “Part of our job as physicians is to help patients and families establish goals of care, process life-threatening events, and, at times, orchestrate the best death possible. We need to embrace this role to the end, allowing relatives the chance to be with a loved one in the last minutes of life, if that is what they desire.”
Against Inviting Family Members to be Present During Resuscitation
James Downar, M.D., C.M., M.H.Sc, drawing on source information from the University Health Network, Toronto, argues against inviting family members to be present during resuscitation.
“My opposition stems from personal experience as a participant in resuscitation teams, when the presence of family members has interfered with the resuscitation efforts. I am concerned that family presence during resuscitation may increase the risk of death for the patient and may also have physical, psychological, or legal repercussions for members of the resuscitation team. Most of all, I am worried about the psychological trauma to a family member witnessing the resuscitation efforts,” Dr. Downar states.
Dr. Downar distinguishes the study by Jabre, et. al. cited by Dr. Kritek — which found less psychological damage to family members who witnessed resuscitation of their loved ones than to those who did not — on the basis that all of the cardiac arrests in that study took place in the patients’ homes, not in an inpatient setting in a hospital. “I hesitate to apply these findings to inpatient resuscitations because cardiac arrests that occur at home are different in that family members actually “invite” EMS to be present for the resuscitation, rather than the reverse,” Dr. Downar states.
“Before generalizing the results of the study by Jabre et al. to the inpatient setting, we need to know more about the mechanisms of harm and benefit that apply when family members are present during resuscitation efforts,” Dr. Downar writes. “Do family members benefit from being present at the resuscitation, or is family presence during resuscitation actually a harm that is mitigated by the presence of a resuscitation team member who provides support during and after the resuscitation?” he asks.
Dr. Downar notes that “not all people react to a given psychological trauma in the same way.” “We need to be careful whom we invite, since some persons may have a predisposition to PTSD after a traumatic event.4 At the time of the event we would have no way to predict which persons are most at risk for PTSD,” he states.
He calls for “further investigation into the effects of family presence during resuscitation in the inpatient hospital setting.”
“But,” Dr. Downar concludes, “until these investigations are complete, I will not routinely invite family members to be present during resuscitation efforts.”
More Information
The Case Vignette, entitled, “Family Presence during Cardiac Resuscitation,” along the Journal’s poll and reader comments, is found in the New England Journal of Medicine, March 14, 2013.
The new study, entitled “Family Presence during Cardiopulmonary Resuscitation,” conducted by Patricia Jabre, M.D., PHD, of the Department of Health Sciences Research at the Mayo Clinic, Rochester, Minnesota, and colleagues, is also found in the New England Journal of Medicine, March 14, 2013. As noted above, this study found that family members present during CPR experienced less anxiety, depression, and PTSD-related symptoms afterward than those who were excluded.
See also press coverage of this issue, primarily discussing the Jabre, et. al. study cited above, for example:
Watching CPR Helps Ease Family’s Grief – MedPage Today
Families May Gain From Observing CPR – New York Times
For more information about heart attack, heart disease and stroke, see the HelpingYouCare® resource pages on Heart Disease & Stroke, including



