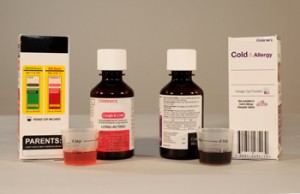
 On May 4, 2011 the U.S. Food and Drug Administration (FDA) issued Ten Tips for Caregivers on How to Prevent Accidental Overdose from Over-The-Counter (OTC) liquid medications, at the same time as the Agency released guidelines to OTC drug companies, aimed at avoiding accidental overdoses resulting from unclear or inconsistent labeling or markings on OTC liquid drug products packaged with cups, spoons, syringes or other devices for taking the medication.
On May 4, 2011 the U.S. Food and Drug Administration (FDA) issued Ten Tips for Caregivers on How to Prevent Accidental Overdose from Over-The-Counter (OTC) liquid medications, at the same time as the Agency released guidelines to OTC drug companies, aimed at avoiding accidental overdoses resulting from unclear or inconsistent labeling or markings on OTC liquid drug products packaged with cups, spoons, syringes or other devices for taking the medication.
Reported accidental overdoses from these products have been increasingly common, and can result from markings on the dispensing devices that are unclear, confusing or inconsistent with labeled dosage directions.
Ten Tips for Caregivers to Prevent Accidental Medication Overdose
The FDA’s Ten Tips to Caregivers on How to Avoid an Accidental Overdose when dispensing these medications were focused primarily on helping parents giving these medications to children, but they apply equally to caregivers dispensing liquid OTC medications, such as liquid pain relievers, cold medicine, cough syrups, and digestion aids, to seniors.
The ten tips for caregivers include:
- Always read and follow the Drug Facts label on your OTC medicine.
- Know the ‘active ingredient’ in the medicine.
- Give the right medicine, in the right amount.
- Talk to your doctor, pharmacist, or nurse to find out what mixes well and what doesn’t.
- Use the dosing tool that comes with the medicine, such as a dropper or a dosing cup.
- Know the difference between a tablespoon and a teaspoon.
- Know your patient’s weight.
- Prevent a poison emergency by always using a child-resistant cap.
- Store all medicines in a safe place.
- Check the medicine three times.
The FDA recommends that anyone with questions about dosage delivery devices or how to measure liquid OTC medicines contact a physician, pharmacist, or other health care professional.
Other Common Medication Errors
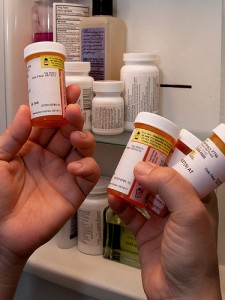 Caregivers should also be aware that due to confusingly similar names of certain medications, or abbreviations used by prescribing physicians, certain prescription medications are known commonly to be mixed up by hospitals and pharmacies, resulting in dispensing of the wrong medication to patients.
Caregivers should also be aware that due to confusingly similar names of certain medications, or abbreviations used by prescribing physicians, certain prescription medications are known commonly to be mixed up by hospitals and pharmacies, resulting in dispensing of the wrong medication to patients.
The FDA maintains a database of reports on such potentially serious preventable medication errors, and provides information and guidance for consumers and caregivers on these common Medication Errors.
This includes a list and information on Drug Products Commonly Associated with Medication Errors. Among those listed that are commonly mixed up:
- Serious medication errors from intravenous administration of nimodipine oral capsules
- Product Confusion with Maalox Total Relief and Maalox Liquid Products
- Dangerous Mix-ups between Insulin and Heparin
- Bumetanide and Norepinephrine
- Serious adverse events and deaths resulting from accidental overdose of high concentration morphine sulfate oral solutions.
- Risk of dispensing errors between KEPPRA (levetiracetam), an antiepileptic, and KALETRA (lopinavir/ritonavir), an antiretroviral
- Reports of medication errors involving confusion between Reminyl and Amaryl (glimepiride)
- Medication errors associated with flomax and volmax
- Medication errors associated with zantac and zyrtec
Caregivers will be well advised to check with your prescribing physician the exact name and spelling, strength, and dosage of the medication being prescribed, and verify with your pharmacist, or the nurse in a hospital, that your senior is in fact getting exactly this medication, with exactly the prescribed strength per capsule or tablet, and per instructions for dosage and administration consistent with those given by the prescribing physician.
If your elder is being given one of the medications listed above, as a caregiver, you should take particular caution to verify that he or she is in fact getting the correct medication.
More information on medications is available as part of the FDA’s Safe Use Initiative, aimed at reducing preventable harm from medication errors.
Disposing of Medications Safely
The FDA also recently issued updated guidelines for consumers and caregivers on how to dispose of unused medications safely.
“Most drugs can be thrown in the household trash, but consumers should take certain precautions before tossing them out,” according to the FDA. “A few drugs should be flushed down the toilet. And a growing number of community-based “take-back” programs offer another safe disposal alternative.”
When disposing of prescription medications, the FDA advises to:
- Follow any specific disposal instructions on the drug label or patient information that accompanies the medication. Do not flush prescription drugs down the toilet unless this information specifically instructs you to do so.
- If no instructions are given on the drug label and no take-back program is available in your area, throw the drugs in the household trash, but first:
- Take them out of their original containers and mix them with an undesirable substance, such as used coffee grounds or kitty litter, to make them less appealing to children or anyone who may intentionally go through your trash.
- Put them in a sealable bag, empty can, or other container to prevent the medication from leaking or breaking out of a garbage bag.
- Before throwing out a medicine container, scratch out all identifying information on the prescription label to make it unreadable. This will help protect your identity and the privacy of your personal health information.
- Do not give medications to friends. Doctors prescribe drugs based on a person’s specific symptoms and medical history. A drug that works for you could be dangerous for someone else. and
- When in doubt about proper disposal, talk to your pharmacist.
For more information, see Safe Disposal of Unused Medicines: What You Should Know
________________________________
See other tips for caregivers in our section on Practical Tips, Skills, Tools & Checklists for Caregivers
_____________
Copyright © 2011 Care-Help LLC



