 The Office of Inspector General (OIG) of the U.S. Department of Health & Human Services released an investigation report on May 4, 2011, finding that among elderly Medicare patients in nursing homes, dangerous antipsychotic drugs are being given predominantly “off label” for conditions such as dementia, for which these drugs have not been approved by the FDA.
The Office of Inspector General (OIG) of the U.S. Department of Health & Human Services released an investigation report on May 4, 2011, finding that among elderly Medicare patients in nursing homes, dangerous antipsychotic drugs are being given predominantly “off label” for conditions such as dementia, for which these drugs have not been approved by the FDA.
The OIG further found that 88% of Medicare claims for these drugs were associated with use for dementia, over 50% of these prescriptions were wrongly billed to Medicare, and 22% were administered by nursing homes in violation of standards set by CMS (the U.S. Centers for Medicare & Medicaid Services).
“In total, 95 percent (nearly 1.4 million) of Medicare claims for atypical antipsychotic drugs were for elderly nursing home residents diagnosed with off-label conditions and/or [dementia],” according to the OIG’s Report.
As explained by the OIG’s report, “After FDA approves a drug to be marketed for a specific use, physicians are permitted to prescribe that drug for other uses. This is commonly referred to as off-label use.” Antipsychotic drugs have not been approved by the FDA for use in treating symptoms of dementia in the elderly, and the FDA has warned that they carry serious and potentially life-threatening risks when used this way.
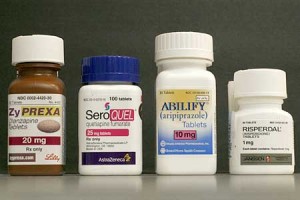
As part of the OIG’s 48 page Report released May 4, Medicare Atypical Antipsychotic Drug Claims for Elderly Nursing Home Residents, the Inspector General attached an Appendix A listing eight commonly prescribed “atypical antipsychotic drugs” and explaining their most common serious side effects. The listed drugs include Aripiprazole (Abilify), Clozapine (Clozaril), Olanzapine (Zyprexa), Olanzapine/Fluoxetine (Symbyax), Paliperidone (Invega), Quetiapine (Seroquel), Risperidone (Risperdal), and Ziprasidone (Geodon).
All of these drugs were approved by the FDA for treatment of schizophrenia and bipolar disorder. Their side effects include a range of conditions, from less serious (e.g. dry mouth) to potentially life-threatening.
Although these drugs were not approved by the FDA for treatment of agitation and other symptoms of dementia/ Alzheimer’s, the government has found that they are commonly being prescribed to the elderly in nursing homes for these conditions.
A 2007 Agency for Healthcare Research and Quality report, referred to in the OIG’s report, listed “the treatment of agitation in dementia” as among the most common “off label” uses of antipsychotic drugs.
The FDA has specifically warned that use of antipsychotics for treatment of dementia in the elderly may create “severe or life-threatening risks.” In April, 2005, the FDA issued a public health advisory that risk of death has been shown to be increased between 1.6 and 1.7 times (i.e. nearly doubled) for elderly patients given antipsychotic drugs to treat agitation and other symptoms of dementia. In fact, FDA required drug manufacturers to place a boxed warning label on these drugs, warning of Increased Morality in Elderly Patients with Dementia-Related Behavioral Disorders, when given these drugs. A sample of such a warning label is included on page 4 of the OIG’s report.
In its Report, the OIG reported that its recent investigation included a review of claims data for nursing home residents over age 65 for whom Medicare claims requesting payment for antipsychotic drugs were submitted to CMS between January 1 and June 30, 2007. For a sample of 600 of these claims, the OIG employed psychiatric medical doctors qualified to prescribe and evaluate the use of antipsychotics, to examine the medical records of the elderly patients.
The investigation found that:
- “Fourteen percent of elderly nursing home residents had Medicare claims for atypical antipsychotic drugs,”..[and] “Claims for elderly nursing home residents accounted for 20 percent of the total 8.5 million claims for atypical antipsychotic drugs for all Medicare beneficiaries during the review period;”
- “Eighty-three percent of Medicare claims for atypical antipsychotic drugs for elderly nursing home residents were associated with off-label conditions; 88 percent were associated with the condition specified in the FDA boxed warning [i.e. dementia];”
- “Fifty-one percent of Medicare atypical antipsychotic drug claims for elderly nursing home residents were erroneous, amounting to $116 million” wrongly billed to and paid by Medicare; and
- “Twenty-two percent of the atypical antipsychotic drugs claimed were not administered [by the nursing homes] in accordance with CMS standards regarding unnecessary drug use in nursing homes.”
As explained by the Inspector General, pursuant to Medicare regulations, “Medicare will pay only for drugs that are used for medically accepted indications approved by FDA or supported by the compendia [the official medical guides for proper prescriptive uses of medications].” The OIG’s medical examiners found that in the investigation sample alone, $116 million of the claims made to Medicare for payment of these antipsychotics given to seniors in nursing homes, violated these regulations.
The OIG explained that, in addition, CMS Standards Regarding Drug Use in Nursing Homes, require that unnecessary drugs not be given to nursing home residents. Nursing homes that violate these standards may not be permitted to participate in Medicare. According to the OIG Report, “CMS defines unnecessary drugs as those that are used:
- in excessive dose,
- for excessive duration,
- without adequate monitoring,
- without adequate indications for use, and/or
- in the presence of adverse consequences that indicate that the dosage should be reduced or discontinued.
As referenced in finding No. 4 above, the OIG found that 22% of the antispychotics administered to residents by the nursing homes in the sample, were not in compliance with these CMS standards. As an example of a failure to comply with these standards, the Inspector General quoted in its report a comment made by one of its medical doctors reviewing the nursing home’s medical records for a beneficiary who received an atypical antipsychotic drug without adequate indications for use: “It clearly seems like [the antipsychotic drug] was ineffective in treating her agitation. Since her agitation was associated with infection and pain, more efforts could have been placed on treating those conditions.”
The Report explains that the nursing homes’ failure to comply with these CMS standards in the administration of the drugs could affect the nursing homes’ ability to participate in Medicare. But under current law, the nursing homes’ faulty administration of the drugs would not void the payment of Medicare claims to the beneficiaries, if the claims were properly submitted for medically accepted uses.
The Inspector General, however, pointed out that under current practice, there is no way for Medicare to determine whether the drug claims are being submitted by the nursing homes, pharmacies or patients for medically accepted uses, without doing a costly independent medical examination of each patient’s medical records. This is because currently no medical diagnosis information is required to be submitted with the Medicare claims.
As a consequence of its findings, the Inspector General made four recommendations for action to CMS:
- “Facilitate access to information necessary to ensure accurate coverage and reimbursement determinations.
- Assess whether survey and certification processes offer adequate safeguards against unnecessary antipsychotic drug use in nursing homes.
- Explore alternative methods beyond survey and certification processes to promote compliance with Federal standards regarding unnecessary drug use in nursing homes.
- Take appropriate action regarding the claims associated with erroneous payments identified in our sample.”
CMS accepted and agreed to act on all of these recommendations, except for the first one. CMS indicated that it cannot comply at this time, since under current practice in the industry, medical diagnosis information is not commonly included in prescriptions and is not available to be verified by CMS. Therefore diagnostic codes are not now required to be included in claims submitted under Medicare Part D. The OIG recommended that diagnostic information should be required to be included, saying:
Enhanced claims data could improve CMS’s ability to enforce criteria for Medicare drug coverage and reimbursement and to determine whether a drug is covered by Medicare. For Part D claims, expansion of the required data elements to include diagnosis codes could help drug plan sponsors and CMS ensure that a drug meets the definition of a Part D-covered drug (i.e., is used for an FDA-approved indication or a medically accepted indication supported by the compendia).
In its response to the report, CMS also specifically stressed concern that contractual arrangements among drug manufacturers and distributors, long-term care facilities, and pharmacies may be causing this problem by providing financial incentives for the improper prescribing of these drugs, adversely affecting the health and safety of residents in long-term care facilities.
Read a summary of the OIG’s report at The HHS Office of Inspector General’s website.
Read the full Report of the HHS Office of Inspector General and the CMS Response: Medicare Atypical Antipsychotic Drug Claims for Elderly Nursing Home Residents
_____________
Copyright © 2011 Care-Help LLC




[...] 2007 report listed “the treatment of agitation in dementia” as among the most common “off label” uses [...]